Apr 4, 2019
A patient presents to the office because of pain in the knee with or without a history of injury. An examination is performed followed by an X-Ray. Osteoarthritis may or may not be seen on the X-ray. If there is an altered range of knee motion when compared to the “normal” side, then a preexisting condition is considered. Whether or not the physician considers arthritis, an MRI is requested. The MRI report 48 hours after imaging is consistent with a torn medial meniscus. Should all patients with a torn medial meniscus undergo surgical intervention? If surgery is undertaken, should the procedure be a repair or a partial removal? The management of meniscal injuries must be influenced by the knowledge that meniscal integrity is important in load distribution across the joint. Meniscal injury causes altered joint mechanics and is related to the onset of arthritis.
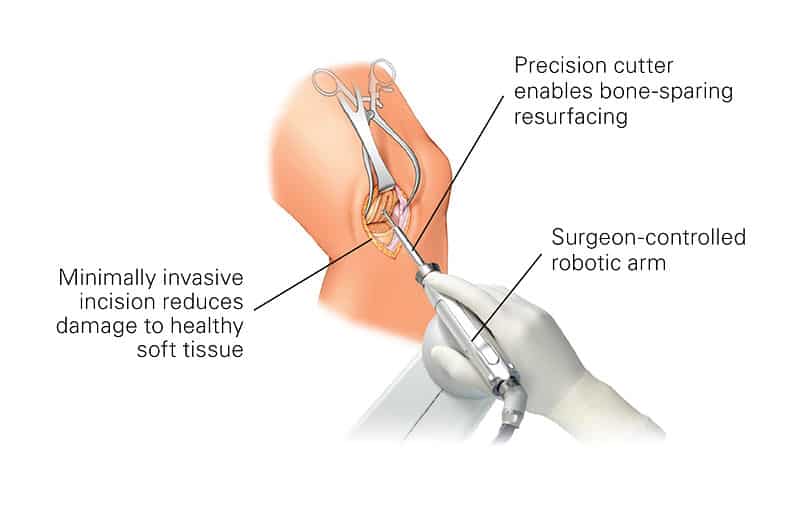
According to a recently published online article in the British Journal of Sports Medicine, arthroscopic partial meniscectomy (APM) may not be the best option for all patients with knee pain and meniscal tear. Researchers investigated patients with meniscal tears that compared Arthroscopic Partial Meniscectomy to nonsurgical intervention, pharmacological intervention, and no intervention. At six to 12 months, APM patients had a slight improvement in knee pain, knee-specific quality of life, and knee function compared to physiotherapy patients. When excluding osteoarthritis (OA) patients, the aforementioned outcomes exhibited small to moderate improvement. Knee pain, function, and quality of life did not improve for APM patients compared to placebo surgery patients at six to 12 months regardless of OA status.
There may, however, be a small-to-moderate benefit from APM compared with physiotherapy for patients without osteoarthritis and who have mechanical or obstructive signs. Arthroscopic partial meniscectomy (APM), a keyhole surgery where loose and fragmented pieces of a torn meniscus is removed, is one of the most common orthopedic procedures performed. Over half of these are performed to treat a meniscus tear in a degenerative knee; however, several recent randomized trials have shown that Arthroscopic Partial Meniscectomy is not superior to conservative treatment or placebo treating meniscus tears associated with a degenerative knee. On the other hand, there is universal agreement that the traumatic meniscus tear, the result of a knee injury in a younger patient with otherwise healthy knee (with no degeneration), should be treated by surgery.
Then what is the downside of meniscal injury and surgery? The medial and lateral meniscus together provide shock absorption, establish a broad base of contact surface and help provide stability to the knee. Those who have undergone total or partial meniscectomy should understand that in five to 15 years, they will develop degenerative arthritis. The long-term outcomes of those whose tears were treated by repair rather than removal has not been established. My Regenerative Medicine practice in part, is the result of those seeking to postpone or avoid a Total Knee Replacement years after a meniscal injury followed by arthroscopic surgery. As long as the arthritis has not progressed to a Grade 4, I am able to assist the patient with joint restoration, at times joint regeneration, it is matter of age and health. While I am able to offer joint restoration, on occasion, joint restoration for those who sustained meniscal and Anterior Cruciate injury in the past, is there anything that could be used as an adjunct at the time of the meniscal injury to promote healing without surgery or postpone, perhaps avoid future postraumatic arthritis?
To learn more. Schedule a consultation (312) 475-1893.You may view my web site at www.sheinkopmd.com.
Tags: ACL, ACL Injury, anterior cruciate, arthritic knee, arthritis, Autologous Protein Concentrate, baseball, BMC, board-certified, Bone Marrow Concentrate, bone marrow edema, cells, cellular orthopedic, cellular orthopedics, FDA, football, golf, Growth Factors, hematopoietic cell, injection, Interleukin 1 Receptor Antagonist Protein, IRAP, joint health, joint pain, knee replacement, lipogems, meniscal injury, meniscectomy, Mesenchymal Stem Cell, micro-fragmented adipose, muscle injury, muscle strain, OA, Orthopedic Surgeon, Osteoarthritis, pain, Physical Therapy, Platelet Rich Plasma, platelets, PRP, regenerative medicine, repair, Rotator cuff tear, soccer, sports injuries, sports medicine, stem cells, strain, tear, torn medial meniscus, training, volleyball

Feb 14, 2019
Following injury or wear, limitations need not be limited to professional, college and high school athletes
Last week, my column focused on the post traumatic ravages of the National Football League season; and getting ready for next cycle of body demolition. Those who watched the championship game saw several players assisted off the field following violent trauma. Even the President announced that he would prefer his son not play football. While professional, college and high school competitive sports enjoy high profile, there are the average recreational sports and fitness enthusiasts who progressively experience a diminution of ability to participate in a sought-after activity by virtue of injury or wear and tear; be it basketball, running, cycling, skiing, hockey, fitness endeavors, volleyball, golf, soccer, sailing; so, on and so forth.
As an example, a 67-year-old man presented in my office last week after having read my column, with progressive pain in his left knee and inability to partake in his long-time recreational passion, volleyball. I completed his intake centered on the taking of his medical history, completed an orthopedic physical examination, and ordered X-rays. He brought a recent MRI study to the appointment. The physical therapist who assists me objectively documented his physical findings so we would have pretreatment measurements. Additionally, my therapeutic recommendation is always based on more than an X-Ray and MRI, but also includes the objective and reproducible Range of Joint Motion and assessment of joint stability.
After review of all the above, I administered informed consent for a Bone Marrow Concentrate intervention into his left knee as a means of postponing, perhaps avoiding a Total Knee Replacement and assisting in his return to recreational volleyball. While there are several options for intervention into the arthritic or injured joint including adipose and blood-based alternatives, I recommended Bone Marrow Concentrate for his moderately arthritic knee as a means of providing Concentrated Platelets, Concentrated Growth Factors, anti-inflammatory Cytokines, Adult Mesenchymal Stem Cells, Precursor Cells, Marrow Adipose Tissue, and Hematopoietic Cells, all consistent with FDA compliance requirements. There are mandatory Federal Drug Administration and Federal Trade Commission regulatory standards of compliance in Regenerative Medicine; patients must be cautious when choosing the minimally invasive Cellular Orthopedic option. It takes an office visit, physical assessment and review of images by a board-certified specialist in the regenerative medicine decision making process; not merely attendance at a seminar. Some patients will not meet inclusion criteria, their needs would be better served by accepted surgical norms.
At age 67, there is little chance at Cartilage Regeneration for my patient, but there is a high probability of Joint Restoration; that is increased motion, diminution of pain and the return of ability, in this patient’s case to play volleyball. He will wear an off-loader brace for six weeks, partake in physical therapy and then gradually return to his Chicago Park District three games a week routine. The patient will have reached his competitive goals through care based on the scientific evidence and outcomes documentation. As long as I introduced the subject of competitive goals, off I go to ski in Colorado next week; about a year after having undergone Cellular Orthopedic interventions to both of my arthritic hips and both of my arthritic knees. Without the biologics, not only would I be unable to ski, I would be ready for two knee replacements and two hip replacements. I should have listened to my mother and stuck to the piano and violin.
To learn more about continuing to reach your competitive goals, visit my web site www.sheinkopmd.com or call and schedule a consultation 312-475-1893).
Tags: arthritis, board-certified, Bone Marrow Concentrate, bone marrow edema, cellular orthopedics, FDA, football, Growth Factors, hematopoietic cell, joint pain, Mesenchymal Stem Cell, OA, Orthopedic Surgeon, Osteoarthritis, Physical Therapy, soccer, sports injuries, sports medicine, tear, volleyball
Jan 24, 2019
Why Should This Blog Matter To You?
- Stem cell treatments are NOT FDA cleared in the United States
- FDA is scrutinizing physicians and centers that are marketing stem cells
Beware of centers that are offering to:
- Relieve pain
- “Regeneration” of tissues
- Avoid surgery
- Treating a variety of inflammatory, degenerative, or autoimmune conditions
Beware of Stem Cells Clinics!
- Many of these “stem cell clinics” are operated by chiropractors or providers that do NOT have a specialty or advanced training in the musculoskeletal system.
- They simply do not have the training necessary to perform these injections nor are they licensed to so do.
- In some cases, surgery is needed. These providers may not evaluate the need for a surgical procedure.
Federal Trade Commission Press Release: https://www.ftc.gov/news-events/press-releases/2018/10/ftc-stops-deceptive-health-claims-stem-cell-therapy-clinic
FTC Court Documents: https://www.ftc.gov/enforcement/cases-proceedings/172-3062/regenerative-medical-group-inc
The Complaint filed by the FTC on October 12th states the following:
Defendant Henderson is aware that the vast majority of amniotic clinical studies in the scientific literature has been conducted on animal models. There are no human clinical studies in the scientific literature showing that amniotic stem cell therapy cures, treats, or mitigates diseases of health conditions in humans, and the medical community considers amniotic stem cell therapy to be an experimental and unproven treatment. (p. 4)
The representations set forth in Paragraph 21 […Defendants have represented…that their stem cell therapy: cures [everything]…Is comparable to or superior to conventional medical treatments in curing, mitigating, or treating specific diseases or health conditions including [everything]…] are false or were not substantiated at the time the representations were made. (p. 21)
The FTC essentially has said that there is no clinical basis to claim a therapeutic benefit to treating patients with amniotic stem cells, so the claims and representations by Dr. Henderson constitute deceptive practices and false advertisement.
If you connect the dots, it would suggest that Dr. Henderson engaged in fraud by taking money from patients and treating them with a preparation for which there is no clinically valid proof of therapeutic benefit. Regardless of whether the Department of Justice gets after him for a criminal complaint of fraud or not, I think organizations that offer up a worthless therapy consisting of amniotic stem cells (until proven otherwise with Level 1 studies) could be good targets for class action lawsuits by defrauded patients. The same situation doesn’t apply to PRP and BMC, (what I do) since there is plenty of clinical evidence of therapeutic benefit including my scientific article published in December, 2018.
Sheinkop, et.al Transnational Medicine – published Dec. 13 2018
A specific protocol of autologous bone marrow concentrate and platelet products versus exercise therapy for symptomatic knee osteoarthritis; a randomized control trial with 2 year follow-up.
If you want to complain to the FDA about having received Amniotic Fluid without benefit, use this link:
https://www.fda.gov/BiologicsBloodVaccines/DevelopmentApprovalProcess/AdvertisingLabelingPromotionalMaterials/ucm118859.htm
Tags: Adult Mesenchymal Stem Cells, amniotic fluid, amniotic stem cells, Bone Marrow Concentrate, Clinical Studies, clinical trial, Clinical Trial. Mitchell B. Sheinkop, Cord blood, FDA, joint pain, joint regeneration, joint replacement, Osteoarthritis, Regenerative, research, stem cell, surgery
Jan 10, 2019
Nonobstructive meniscal tears
There is increasing evidence to suggest that patients with meniscal tears at the knee that do not cause “clunking”, giving way, or locking; hence nonobstructive, may benefit from Cellular Orthopedic intervention coupled with physical therapy. Previous studies involving patients over 45 years of age comparing arthroscopy with physical therapy for nonobstructive meniscal tears as seen on an MRI justify an initial conservative approach; but patient satisfaction may require 24 months to achieve. For those patients who undergo arthroscopic surgery, there is a significant increased risk of repeat knee surgery. In our practice, those patients electing to use the Physical Therapy option without surgery but with a Cellular Orthopedic intervention minimized the length of time needed to return to full activity.
Number of stem cells in amniotic fluid
The functionality of stem cells in amniotic fluid as sold today is a myth. Research shows that 250cc of fresh C-section delivered amniotic fluid, when introduced immediately into culture, only yields 40 stem cells. This means there are 0.16 stem cells per 1 cc of full-term amniotic fluid. Scientific literature referred to by the amniotic fluid marketing forces is based on amniotic fluid collected early in pregnancy.
Acetabular Labral Tear
A hip (acetabular) labral tear is damage to cartilage and tissue in the hip socket. In some cases, it causes no symptoms. In others it causes pain in the groin. Just because a tear is seen in the hip labrum on an MRI, it does not mean the tear is necessarily the cause of the pain. Before initiating treatment, the orthopedic surgeon must exclude that an underlying arthritic condition within the hip is not the real pain generator. More recently recognized is predisposition for a tear in those with abnormal acetabular architecture.
On biologics for knee osteoarthritis
Orthobiologics may become a mainstream treatment for knee osteoarthritis. While Platelet-rich plasma and hyaluronic acid injections are the most established biologics-based treatments for knee osteoarthritis so far, it’s not too early to make confident use of stem cells. At the same time, I must continually warn patients to be particularly careful about claims for these substances. All recommendations for intervention must be FDA compliant and evidence based. (To learn about my contributions to the cellular orthopedic scientific evidence, visit www.sheinkopmd.com. Under the information bullet on the top, you will find published articles)
Eventually, I believe the science and FDA will triumph over quackery and orthobiologics will become an essential part of every knee surgeon’s armamentarium. Available orthobiologics, include:
- Hyaluronic acid
- Platelet-rich plasma
- Cytokine modulation
- Stem Cells
- Exosomes
- Adipose tissue
To learn more or to schedule an evidence based consultation, call (312) 475-1893
Tags: adipose tissue, amniotic fluid, biologics, bone marrow, cytokine modulation, Exosomes, fat, hyaluronic, joint, labral tear, Micro-Fractured Adipose, orthobiologics, Osteoarthritis, pain, Platelet Rich Plasma, PRP, renovation, stem cell, torn meniscus
Dec 5, 2018
As interest in biologic therapies for arthritis-a needle, not a knife-continues to expand; patients increasingly are turning to the ads in newspapers or searching the Internet to gather information on this topic. While there is still a lack of scientific consensus on the use of biologics, it is most important for those seeking information not to be misled. My own analysis of resources for patients seeking on line information about biologic therapies for arthritis is that the overall quality is very poor and anything but scientific. Even worse, is a seminar, neither a reliable or credible source of scientific evidence.
Biologic therapies consist of stem cells, platelet rich plasma product and bone marrow aspirate concentrate. New research, I co-authored and that was published last month in The American Journal of Orthopedics: Safety and Efficacy of Micro-Fractured Adipose Tissue for Knee Arthritis, is indicative of the ever-evolving nature of Regenerative Medicine. Biologic therapies and their use in arthritis or musculoskeletal injury in general are an area of vast research and interest within the medical field. Understanding the information online and the misinformation provided at seminars pertaining to biologics allows me to tailor my conversation and address commonly found inaccuracies.
The use of Biologic Therapies is expected to significantly increase in the coming years as our knowledge advances on the use of such. That initiative will be led by well informed, well-educated Board Certified, and Fellowship trained specialists. Unfortunately owing to the relative lack of oversite at present, every type of charlatan, parasite and camp follower can buy an ad for a seminar or produce a web site on the internet. How then should a patient with pain and limited function from arthritis seek to postpone or avoid surgery without becoming a victim of the cord blood or amniotic fluid hoax?
- Your physician must complete a comprehensive medical history, physical examination and review of diagnostic studies.
- Explain the disease process and grade of progression,
- Discuss possible treatment options,
- Present a balanced assessment of the current scientific evidence.
Woe, while writing this Blog, I was just notified about acceptance of yet another scientific article by a peer reviewed medical journal in which I am the senior author: A Specific Protocol of Autologous Bone Marrow Concentrate and Platelet Products Versus Exercise Therapy for Symptomatic Knee Osteoarthritis; a Randomized Control Trial with 2 Year Follow-up.
Hopefully some time soon, a Biologic Arthroplasty will be possible; but until then, a Total Joint Replacement is still a necessary option for those not meeting specified inclusion criteria for biologics. To see what treatments may be possible for your arthritic generated pain call (312) 475-1893 to schedule a consultation. Visit my website www.SheinkopMD.com for additional information.
Tags: Adult Mesenchymal Stem Cells, amniotic fluid, ankle pain, arthritic pain, autologous bone marrow concentrate, biologic, biologics, cellular orthopedics, Cord blood, Hip pain, injury, joint pain, knee pain, lipogems, Osteoarthritis, PRP, regenerative medicine, rupture, shoulder pain, sports injury, stem cell, tear, tendinitis
Aug 16, 2018
From the front page of the September, 2018 issue of GOLF “This Tiger is for real. He’s faster, sharper-and an up-and-down machine.” Then, from the September/October issue of Tennis, “Juan Martin del Potro He’s back…. and ready to once again conquer”. His once promising career was reaching the end owing to wrist injuries. Quoting Del Potro in the article “one doctor would say something to me; another would say something different. It was difficult to believe one or the other”; however, he demanded excellence and eventually found it
I could go on citing and quoting from all sports and recreational resources but you get the idea. These are recovery and come back examples of what motivated individuals may accomplish. Now, if you tune in to upcoming US Open later this month, you will be able to follow Rafael Nadal, another super athlete who was able to return to compete at the top of his game owing to cellular orthopedics for several potentially career ending injuries over recent years. I could go on with the examples in each and every recreational pursuit or from those who wished to regain a pain free and very active life even if not at the aforementioned level of demand. Suffice it to say, the common denominator for those with skeletomuscular restrictions is a combination of physical training, mental motivation and timely medical care.
You can put some of this Tiger in your tank and reignite your enjoyment of activities at any level if arthritic or traumatic injury of your bone and joints is holding you back. The new world, (actually it is not so new anymore) of Cellular Orthopedics may allow for a return to a virtually unlimited lifestyle with a needle instead of a knife. I choose to define myself as a Cellular Orthopedist so a patient might not be trapped in the web of so called regenerative medicine specialists. An orthopedic surgeon has dedicated many years to understand the musculoskeletal system whereas a regenerative medicine clinic frequently is populated by those who attended a two-day training seminar. While my own recreational pursuits and fitness profile is far removed from those of the famous professionals noted earlier in this blog, following cellular orthopedic interventions into my own knees in December of 2017, and for my hips in January, 2018, I returned to skiing last winter, cycling and fly fishing this summer, and I am able to enjoy a full fitness commitment in doing my part to maintain the highest possible level of performance.
You may access my website at WWW.SheinkopMD.com or call (312) 475-1893 to schedule a consultation.
Tags: BMC, Bone Marrow Concentrate, cellular orthopedis, golfers elbow, injection, Platelet Rich Plasma, PRP, regenerative medicine, sports injury, stemcell, tendon repair, tendon tear, tennis elbow



