
Jun 22, 2020
“They are close to reaching the max number in the study and feel they have enough data at this point.”
While we still could offer adipose derived stem cells to patients via Liposuction and processing of the adipose tissue to recover millions of stem cells, the procedure will revert to fee for service. In the post PSC Trial treatment protocol, it would be possible to address several joints in the same setting with adipose derived cells. Owing to the changes in the PSC Trial protocol necessitated by the COVID-19 virus mandated quarantines, the FDA has diminished the number of patients needed to be enrolled. While I have not yet harvested the adipose tissue from all current enrollees, nor have I injected the stem cells in those already having gone liposuction, we will be done harvesting and delivering the stem cells by mid-summer and have done our part.
Personalized Stem Cells Trial Update
At the beginning of the Trial last August, PSC became the first FDA approved clinical trial in the United States allowing the seven investigative sites to create a drug from a patient’s tissue for the treatment of arthritis. As it stands now, all biologics will be reclassified as drugs by the FDA as of November, 2020 and Personalized Stem Cells became the leader in this endeavor. It will not be for another six months that our team of seven clinical trial sites will have the necessary outcomes data required which would allow the FDA to reclassify the stem cells recovered from your adipose tissue as an approved drug.
On another note, yesterday, Northwestern Memorial Hospitals announced a “successful double lung transplant” to treat a young patient whose lungs were destroyed by the the COVID virus. In a previous Blog, I had introduced the PSC initiative to treat COVID pneumonia with adipose derived stem cells. That trial is underway in San Diego. One of the advantages enjoyed by those who are enrolled in the knee arthritis trial is storage of their stem cells. Those stored cells are available to enrollees for the future care of an arthritic joint in addition the study knee; but as well, for systemic disease outside of the musculoskeletal system such as COVID pneumonia. There are stem cells harvesting and storage companies cropping up on the internet; but as of this time, only Personalized Stem Cell, Inc.is allowed to treat. Should this pandemic continue, a patient at risk, be it age related or health related, for COVID complications just might contact our office and arrange for a fat graft harvest and storage of those adipose derived stem cells to meet a future need.
To schedule a consultation for the care and treatment of your symptomatic joint with limited function, call (312) 475-1893. You may visit my web site and watch my Blog at www.sheinkopmd.com To learn more about Personalized Stem Cells and the COVID lung trial, visit PersonalizedStemCells.com
Tags: clinical trials, personalized stem cells, stem cell clinical trial

Feb 11, 2020
This past Sunday morning, I was reading the Chicago Tribune sports section to learn about the pundits’ opinions regarding the basketball game played by Duke and North Carolina on Saturday night, one of the most amazing basketball games I have ever seen, (incidentally, Auburn versus LSU was great, as well) when I came across the Golf Headline “Mickelson’s short game pays off big”. Why my interest? Phil Mickelson has psoriatic arthritis controlled by TNF-Alpha blocker, a Growth Factor. Another golfer whose career was restored by Growth Factors is Tiger Woods. In Woods’ case, he had received Platelet Rich Plasma (PRP) with Growth factors; Platelets produce those biologic agents. Then there is the story of Kobe Bryant, who had traveled to Germany in 2012 to extend his professional career for seven years with Interleukin One Receptor Antagonist Growth Factors recovered from circulating blood. At the time, Bryant travelled to Germany, the treatment he was to receive was not FDA approved in the United States. There is now an innumerable list of professionals and amateurs who have returned to the game or prolonged a career through Growth Factors thanks to the recreational impact of biologics.
If you surf the internet for Regenerative Medicine and Biologic alternatives, you encounter the term “Stem Cells”. The reality is that as of this time, there is no FDA or legal way to avail yourself of Stem Cells alone; the only access is by concentrating your bone marrow and injecting the concentrate into the arthritic joint since there are Adult Mesenchymal Stem Cells in your bone marrow.
Concentrated Platelets, Growth Factors, and Concentrated Bone Marrow have been the regenerative and restorative mainstays in my practice until now.
Looking to the future, because I have been involved with several Cellular Orthopedic Clinical Trials over the past five years, my practice is assisting in the creation of pathways for yet another biologic trial in 2020. Most exciting is the FDA approved Personalized Stem Cell Clinical Trial in which ours is one of seven designated and FDA approved centers. The PSC FDA-approved Clinical Trial was launched in August of last year. In September of 2017, the FDA warned that by November of 2020, all biologics would be reclassified as drugs. Personalized Stem Cells was granted FDA approval to create a drug from your own adipose tissue. The abdominal fat is recovered by Liposuction and processed in a facility that has met all FDA and Good Practice Management governmental requirements. The resultant Stromal Vascular Fraction (Stem Cells recovered from fat) number in the tens of millions and are made available for injection into an arthritic knee. You may learn more at WWW.PSC.Com or on my web site www.SheinkopMD.com. To schedule an appointment or consultation, call (312) 475-1893
Tags: biologics, orthobiologics, recreational impact of biologics
Dec 17, 2019
The progress in the emerging discipline, Orthobiologics, in part, is the result of the FDA and FTC taking on a stronger oversite role; but additionally, the data I gather contributes to these scientific advances. I will elaborate in this blog.
In order to be FDA compliant, the use of stem cells must be autogenous; that is, the cells must come from you. The orthobiologic industry finally complied so those providers with integrity have made available acellular growth factors. Three weeks ago, I learned that is some cases, Medicare and certain insurance companies will preauthorize said usage. Stay tuned on this one as to whether the product works and whether its use is indeed reimbursed.
Last week, I was made aware that the FDA had served notice to Chara Biologics and Liveyon for marketing biologic products that are unapproved. Stay tuned as more bad actors will be shut down.
https://www.fda.gov/news-events/press-announcements/fda-sends-warning-companies-offering-unapproved-umbilical-cord-blood-products-may-put-patients-risk
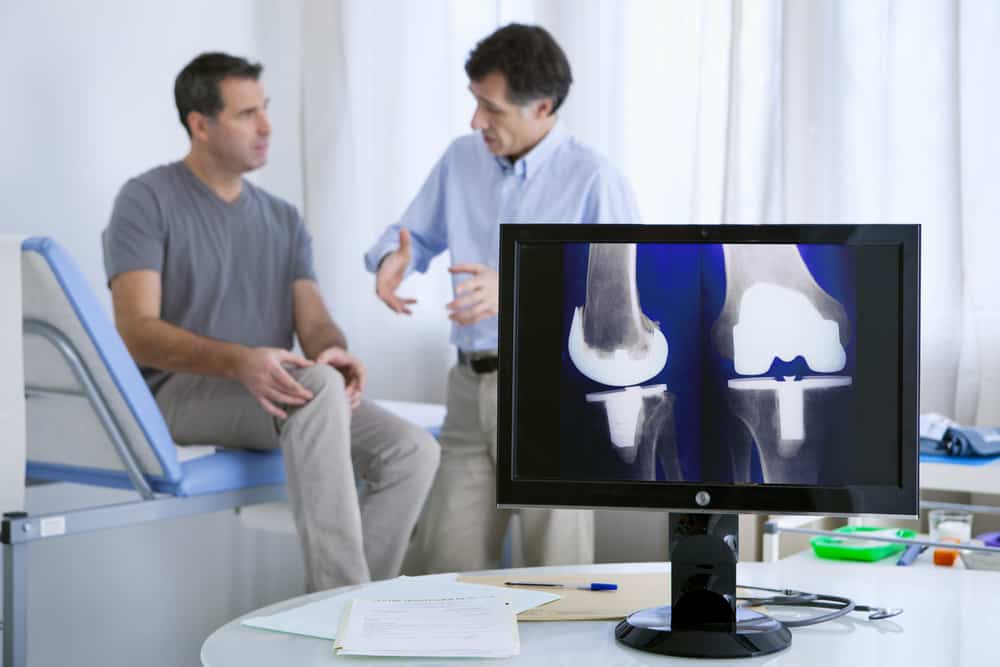
Biologic Interventions to Avoid Joint Replacements
This past Friday, I received biologic interventions into my right and left hip and my right and left knee. It worked for me two years ago and I believe the biologics will help postpone, maybe avoid joint replacements while allowing me to keep skiing, fly fishing, cycling, and keeping fit. There were no appreciable amounts of stem cells in that which was processed from my own blood and injected. The anticipation is that the Platelets and Growth Factor Proteins will diminish the pain of arthritis, and assist in restoring full motion to my hips and knees, allowing me to continue my recreational profile.
In the presence of a single arthritic knee joint, I would have enrolled in the FDA approved Personalized Stem Cell Clinical Trial. You may learn about the Trial at www.Personalizedstemcells.com or on my web site at www.sheinkopmd.com. In the upcoming months, it is hoped that the FDA will expand approval of the PSC Trial to both knees and eventually, the hips. At this time, there are only two FDA compliant methods of allowing physicians to provide a patient with “stem cells,” one is via your bone marrow and the other via your adipose tissue. In my case, with the several joints involved and given realistic outcome possibilities, I opted for the Growth factor approach. My next step will be the Stem Cell option.
I will be testing my outcomes of the Biologic interventions next week on a bone fishing trip four-five days in Punta Allen, Mexico. While my schedule is full prior to departure, there are still some office openings available on Tuesday, December 31. To schedule an appointment at any time call (312) 475-1893
Tags: biologic intervention, orthobiologics, regenerative medicine, stem cell research, stem cell trials
Nov 26, 2019
This past Saturday and Sunday, we had the pleasure of hosting our nephew and grandniece during a college visit. The nephew is a 52-year-old extremely athletic man who initially had complained of pain and swelling in his left knee ten years ago. At the time, he had sent me his MRI imaging, the latter compatible with a partial tear of his lateral meniscus and a cartilage defect in his lateral femoral condyle. Both the local orthopedic surgeon and I advised a wait watch and see approach since the problem was not mechanical but rather inflammation leading to pain and swelling. After a single cortisone injection, physical therapy, and three months, the problem resolved. Ten years later after a soccer match, my nephew presented with recurrence of symptoms. While there still are no mechanical signs such as instability, clunking, giving way or locking; whereas ten years ago, he had no asymmetry in his range of motion, he now had a loss of full extension and full flexion. These latter two are the signs of osteoarthritic changes. Before advancing a treatment program, I asked him to complete a new set of images including an X-Ray and MRI.
It is more probable than not that the imaging will be compatible with grade 3 osteoarthritic changes where the lateral femoral articular defect had been initially seen associated with the lateral meniscal tear. The altered range of joint motion tells the story. What follows is my informed consent.
Cortisone has a short-term anti-inflammatory effect. We have learned it has a probable systemic effect as well as intraarticular since diabetics experience an increase in their management needs for up to 72 hours following the injection into a joint. The second option is a hyaluronic acid injection. While the latter may provide up to six months of pain relief in 60% of patients, the inconsistencies in patient response have led to an ever-increasing refusal of preauthorization by Medicare and private indemnifiers. What about the arthroscopic surgical option? Orthopedic surgeons have increasingly abandoned the notion of surgical cartilage restoration and joint preservation because of inconsistent or short-term success at best.
Is there any chance of postponing, perhaps avoiding a joint replacement, either total or partial? The answer to the question is why I “graduated” from joint replacement to the new discipline of Cellular Orthopedics or Orthobiologics. The attempt to relieve pain, improve function, restore motion, stop the progression of osteoarthritis with a needle instead of a knife is based on cells, platelets and proteins, the latter known as Growth factors. In order to be FDA compliant, the cells and platelets must be autologous; that is, they must come from you. While it is also most desirable and effective to use Growth Factors from your bone marrow or circulating blood, recently, Medicare and some private insurance carriers have preauthorized amniotic fluid as long as it is produced for pain relief and as a source of Growth Factors but, without stem cells. Returning to my nephew’s problem, is there the possibility of cartilage regeneration or is the goal, joint restoration?
As space is limited for posting my blog, you will have to “tune in” next time to learn more. In the meantime, to schedule an office consultation, call (312) 475-1893. You may watch my webinars by visiting my website at www.sheinkopmd.com and clicking on the Webinars dropdown menu.
Nov 1, 2019
Two Fridays ago, I spent my day developing two new webinars so my patients, present and future, will be informed and updated. While the ultimate regenerative educational experience will take place at the time of an office visit and consultation, I believe the best patients are those most informed. The webinar concerning the FDA approved Clinical Trial for creating a new drug termed Stromal Vascular Fraction out of your adipose tissue recovered during a mini-liposuction, is already accessible on my web site at sheinkopmd.com; here is a link to review my newly produced webinar for the primary joint restorative and regenerative procedures that I do: https://www.youtube.com/watch?v=rzfkdzKJ9j8&feature=youtu.be
You will note in the latter, an overview of all the procedures that I use in my practice, all are evidence-based and FDA compliant. I am one of a handful of cellular orthopedic surgeons who have substituted a needle for a knife in an attempt to assist a patient in postponing, perhaps even avoiding a major surgical procedure for an arthritic joint.
It is difficult for the reader and viewer to realize the time and effort involved in practicing evidence-based regenerative medicine; the much easier approach is an anecdote and a bill. Below I will share an edited abstract of the latest abstract that I am submitting to an Ortho Biologic meeting and shortly thereafter, to a major scientific journal for publication.
Title: Minimum 12-month Clinical Outcomes of a Combined Intraosseous and Intraarticular Treatment of Knee Osteoarthritis with Autologous BMC
ABSTRACT
Purpose: To summarize safety and outcomes in a clinical study in which study subjects with knee osteoarthritis (OA) were treated with a bone marrow concentrate (BMC) preparation who received a split treatment of autologous BMC implanted intraosseous into the tibial plateau and intraarticular.
Conclusion: Study subjects tolerated the outpatient procedure, performed with conscious sedation, reporting only mild discomfort resolving within 2-3 days post-procedure. The combined intraarticular/intraosseous BMC therapeutic approach appeared to provide moderate to significant pain relief and improvement in functional scores for 80% of the patients (KSS-Knee, LEFS and VAS). All study subjects have remained in the study as of an average of 1.5 yrs post-treatment.
To learn more visit my website at sheinkopmd.com.
To schedule an appointment for the consultation call (312) 475-1893.
Jul 30, 2019
In my last blog, I announced the approval by the FDA for a new drug application allowing use in treating knee arthritis. Personalized Stem Cells, Inc (PSC) a human adipose-derived stem cell company, received the FDA approval allowing use of a person’s own adipose-derived stem cells to treat osteoarthritis. The first clinical trails will begin in August. I am thrilled to announce that I have been chosen as one of the investigators
Personalized Stem Cells, Inc (“PSC”), a human adipose-derived stem cell company, has received FDA approval for a New Drug (IND) application for use of a person’s own adipose-derived stem cells to treat their osteoarthritis. The first clinical trial, expected to begin in August, uses stem cells as a treatment of osteoarthritis in the knee.
This is the first of several planned clinical trials which will enable qualified PSC-enrolled physicians to provide FDA compliant, regulated quality cell therapy to patients suffering from osteoarthritis. PSC plans to conduct a series of FDA approved clinical trials starting with uses in orthopedics and expanding to other medical conditions in the future.
PSC is working with the FDA to provide alternatives to unregulated, in-clinic stem cell processing and unapproved “regenerative” therapies. The current environment of in-office, unregulated manufacturing of stem cells by physicians has come under serious regulatory action by the FDA, FTC, and the Federation of State Medical Boards. It is clear that the only allowed use of stem cells will be through legitimate FDA clinical trials with manufacturing in a controlled FDA inspected, GMP compliant facility.
PSC was founded by Robert Harman, DVM, MPVM and Michael Dale, both of whom also co-founded VetStem Biopharma and are both experienced serial entrepreneurs.
“This first clinical trial will not only provide an approved method for treatment of knee arthritis, but it will also demonstrate that it is possible to work within the FDA regulatory guidelines to bring advanced stem cell therapy to the public. We have made remarkable progress in obtaining our first approval in less than one year after forming the company,” says Mr. Dale.
PSC has enrolled a limited number of clinical sites around the U.S. to provide treatment of knee osteoarthritis using stem cells. The physicians in this first clinical trial are among the most experienced stem cell physicians in the country. Contact PSC for clinical trial information, clinical trial site locations, or investment information.
Personalized Stem Cells was formed in 2018 to advance and legitimize human regenerative medicine. This privately held biopharmaceutical enterprise, based near San Diego (California), offers qualified physicians who enroll, an FDA compliant autologous stem cell product (from patient’s own fat tissue) for use in FDA approved clinical trials. PSC is driving development and adoption of stem cell and regenerative medicine within the FDA-IND process by providing quality manufactured, safety tested cells, and well-defined clinical trials. PSC has licensed a portfolio of over 70 issued patents in the field of regenerative medicine. For details regarding this first study, visit https://personalizedstemcells.com/clinical-trials/current-clinical-trials/
For more information regarding the trial call 1(312) 767-5761. You may schedule an office visit by calling (847)390-7666 or visit my web site at sheinkopmd.com


